
Poor sleep triggers hormonal changes that make your body more insulin resistant.
Poor sleep spikes cortisol. Cortisol makes you insulin resistant and tells your liver to dump glucose. Growth hormone gets disrupted. Inflammatory markers go up. Your sympathetic nervous system stays more active.
Studies show that even one night of 4-5 hours of sleep can reduce insulin sensitivity by 20-30% the next day. Deep sleep is when your body does metabolic repair work. Growth hormone gets released properly. Cortisol drops. Your cells become more responsive to insulin.
People who sleep well consistently need less insulin for the same food. Their basal rates hold steady. Corrections work predictably.
High blood sugar overnight wakes you up to pee and disrupts deep sleep. Low blood sugar triggers adrenaline and cortisol, which wrecks sleep quality.
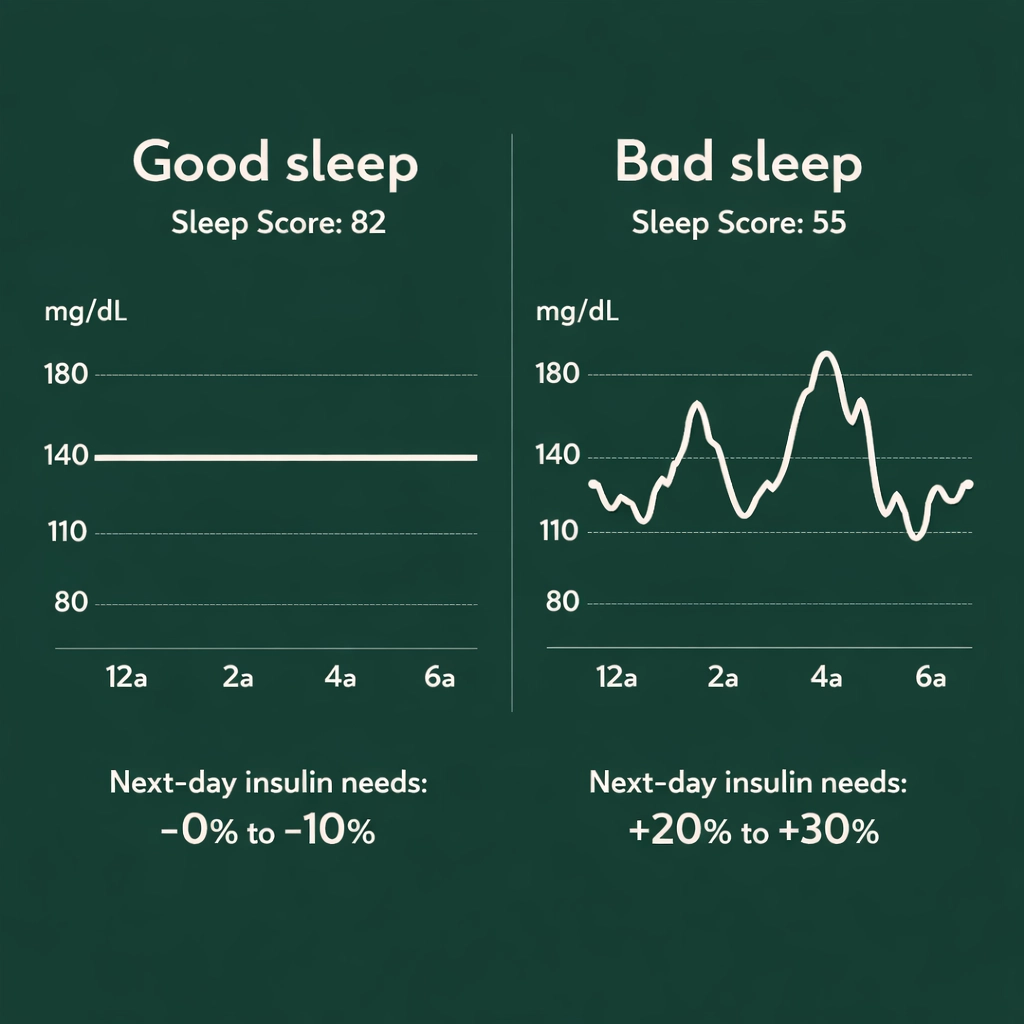
Poor sleep makes you more insulin resistant the next day, which makes blood sugar harder to manage, which makes the next night worse. After poor sleep, most people need 20-30% more insulin the next day.
After several nights of good sleep, insulin sensitivity improves. The same doses that barely worked suddenly become adequate or too much. The difference between well-rested and sleep-deprived can mean needing 30 units per day vs 40 units for the exact same food and activity.
Going to bed with stable blood sugar (roughly 110-140 and flat) reduces overnight interruptions. Consistency helps. Same bedtime, same wake time.
But even with perfect diabetes management, a bad night makes the next day harder. And even with chaotic blood sugar all day, good sleep can reset things by morning.
Sleep isn't optional for good diabetes management. It's foundational.