
Type 1 diabetes is a weird version of The Hangover.
You wake up in a location: except instead of Vegas or a tiger in your bathroom, it's a blood sugar number. And you have no idea how you got there.
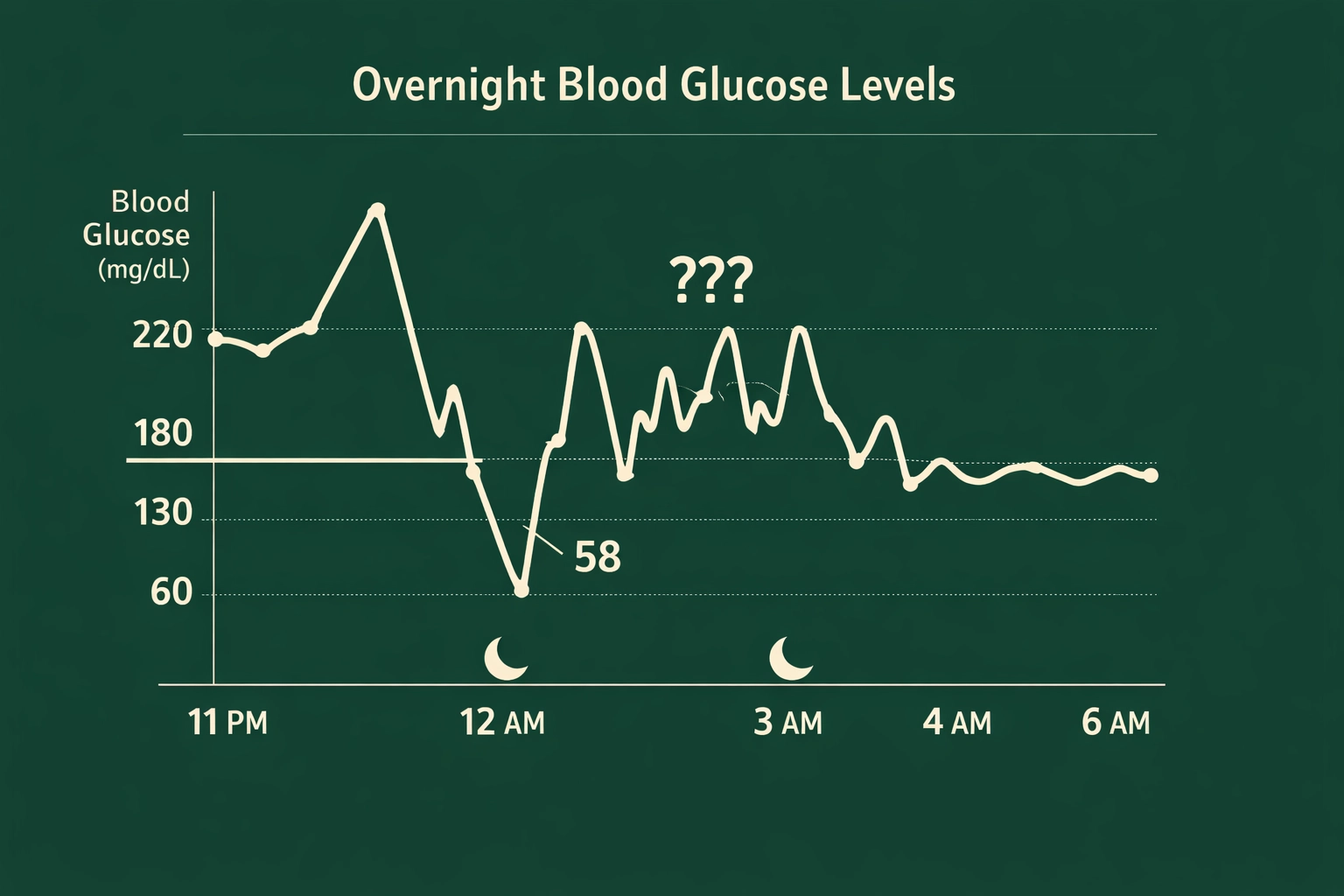
You went to bed at 130. Stable. Perfect graph. You wake up at 220.
Or worse: you went to bed at 130 and wake up at 58 with that lovely shaky feeling and your heart trying to escape your chest.
The question is always the same: What the hell happened between 11pm and 6am?
Bedtime with Type 1 isn't "brush teeth, read a bit, lights out."
It's a whole situation.
Check CGM. Are you stable? Trending up? Trending down? Is that arrow flat or just pretending to be flat before it decides to nosedive at 2am?
You're 140 and rising. Do you correct now? How much? Too much and you'll crash at midnight. Too little and you'll wake up at 250.
You're 90 and flat. Seems fine. But is it actually flat or is it about to drop? Should you eat something preventatively? How many carbs? Do you bolus for it? (Probably not, but now you're thinking about it.)
You're 170 and flat. High enough that you want to bring it down. But will that correction hit too hard overnight when your insulin sensitivity changes?
Every single night is a probability calculation you don't have enough information to solve.
So you guess. You make your best call. You get in bed.
And then you wait.
Here's what nobody tells you about overnight blood sugar management: you never really stop managing it.
Even if you don't set an alarm, your brain does it for you.
You wake up at 2am. Not because your CGM alarmed. Just because some part of your brain decided to check in. You grab your phone. 110 and flat. Great. Back to sleep.
Except now you're awake. And you're thinking about it. And maybe that graph isn't as flat as it looked. Maybe that's the start of a rise. Maybe you should check again in an hour.
You don't go back to deep sleep after that.
Or worse: you wake up at 2am and you're 68. Now you have to get up. Stumble to the kitchen. Eat glucose tabs or drink juice or eat whatever's fastest. Then sit there and wait for it to come up because going back to bed at 68 feels like tempting fate.
Twenty minutes later you're 95 and rising. Good. Back to bed. But now it's 2:30am. You've been awake for 30 minutes. You're not getting that deep sleep back.
And in three hours you might wake up at 180 because you overshot the low.
Sometimes you don't even make it to 2am.
You're lying there. Eyes closed. Trying to sleep. And you feel it. That slight off feeling. Not dramatic. Just... something.
You check. 75 and trending down.
Dammit.
Now you have to eat. You don't want to eat. You're not hungry. You brushed your teeth. You were almost asleep. But you have to eat because if you don't, you'll be 50 in an hour and then you'll really be awake.
So you eat something. Glucose tabs if you're disciplined. Crackers if you're human. Half a cookie if you're tired and annoyed.
Then you wait. Check again. Still dropping. Eat more. Check again. Finally starting to come up.
By the time you're back in range and actually trending stable, it's been 40 minutes. You're fully awake now. And you just consumed 30 carbs you didn't need or want.
The next morning your time-in-range report shows a beautiful flat line at 110 all night.
Nobody sees the three interruptions it took to get that line.
Morning comes. You open your eyes. First thought: where am I?
Not literally. You're in your bed. You know that.
But blood-sugar-wise? No idea.
You grab your phone. The number loads.
Or you wake up at 62. Also confusing. You had a snack before bed specifically to prevent this. But here you are anyway.
The worst part isn't the number itself. It's the not knowing.
You retrace your steps like you're trying to solve a crime. What did I eat yesterday? When did I last change my site? Did I sleep poorly? Was I stressed? Did I bolus correctly at dinner?
Sometimes you can piece it together. Usually you can't.
You just woke up at a blood sugar level with no clear explanation of how you got there.
The Hangover. But every single night.
Your body does a lot overnight that has nothing to do with what you ate or how much insulin you took.
Cortisol rises in the early morning (dawn phenomenon). Growth hormone gets released during deep sleep. Your liver can decide to dump glucose for reasons known only to itself. Your insulin sensitivity changes between midnight and 6am.
Basal rates try to account for this. Sometimes they work. Sometimes they don't. Sometimes they work Monday through Friday and then stop working on Saturday for absolutely no reason.
And if you don't get deep sleep: because you're waking up to check your CGM or treat a low or pee because you're high: then your cortisol and growth hormone are even more chaotic, which makes insulin sensitivity worse, which makes the next night worse.
It's a cycle that feeds itself.
The numbers are annoying. The interruptions are annoying.
But the real cost is the sleep you don't get.
Not just the quantity. The quality.
You can be "in bed" for eight hours and still wake up exhausted because you never got more than 90 minutes of uninterrupted deep sleep.
Your body was busy managing a chronic condition all night. Your brain was on call. Even when you didn't wake up fully, you were half-monitoring. Never fully off.
And that adds up.
Day after day of mediocre sleep makes everything harder. Insulin sensitivity tanks. Decision-making gets worse. You're more irritable. You're hungrier. Your body is more inflamed.
Which makes blood sugar control harder. Which makes sleep worse. Which makes control harder.
Most people with Type 1 can't remember the last time they woke up fully rested.
Here's what gets me: people talk about diabetes management like it's a daytime job.
Count carbs. Dose correctly. Exercise. Check your numbers.
All of that happens when you're awake and actively managing.
But eight hours a day: a third of your life: you're supposed to be unconscious. And your diabetes doesn't stop. It just keeps going. And you're either interrupting your sleep to manage it or you're rolling the dice and hoping you wake up in a reasonable location.
There's no opt-out. There's no "I'll deal with this in the morning."
Your body is doing stuff all night. You have to respond to it. Or at least be ready to respond to it.
That's the part that's exhausting in a way that's hard to explain to someone who doesn't live it.
It's not dramatic. It's not an emergency. It's just this quiet, constant thing that never fully turns off.
You go to bed wondering where you'll wake up.
And every morning, you find out.